
A Complete Overview of Hiatal Hernia
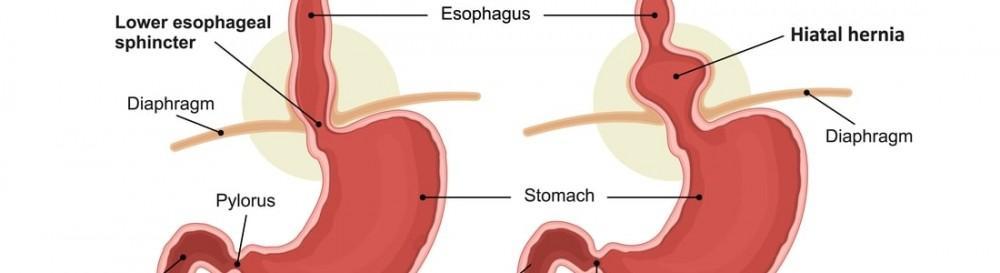
A hernia is a condition in which an internal organ of the body projects out through the wall of the muscle or the tissue that contains it. A hiatal hernia is one of the most common types of hernia. It occurs when the upper part of the stomach protrudes through the diaphragm – it is a large muscle sheet that separates the chest cavity from the abdomen. There is a small opening in the diaphragm that is called hiatus and the esophagus passes through this opening where it connects to the stomach. When a hiatal hernia occurs, the stomach pushes up through hiatus into the chest cavity.
If the hiatal hernia is small, it doesn’t cause any problem unless the doctor discovers it while checking the patient for another health condition.
If the hiatal hernia is large, it allows the food and stomach acid to back up in the esophagus and this causes heartburn. Normally, medications and self-care measures help to manage these symptoms. But, surgery might be needed if the hiatal hernia is very large.
Read on further to know the types, symptoms, causes, risk factors, diagnosis and treatment of hiatal hernia:
WHAT ARE THE TYPES OF HIATAL HERNIA?
There are two main hiatal hernia types:
- Sliding hiatal hernia
- Paraesophageal hiatal hernia
SLIDING HIATAL HERNIA:
In this type, the stomach and the segment of the esophagus that connects the stomach slide up into the chest through the hiatus. This is the more common type.
PARAESOPHAGEAL HIATAL HERNIA:
This type is less common but is more of a concern. The esophagus and the stomach stays in their usual sites, but part of the stomach squeezes through the hiatus and stays following the esophagus.

WHAT ARE THE SYMPTOMS OF A HIATAL HERNIA, WHEN SHOULD THE PATIENT SEE THE DOCTOR?
Usually, small hiatal hernias don’t cause any sign or symptom. But large hiatal hernias cause these symptoms:
- Heartburn
- Abdominal or chest pain
- Having difficulty in swallowing
- Food or liquids regurgitate into the mouth
- Acid reflux (stomach acid backflows into the esophagus)
- Shortness of breath
- Vomiting of blood or passing the black stools, which may show gastrointestinal bleeding
The patient should see the physician when the signs or symptoms are persistent.
WHAT CAUSES A HIATAL HERNIA?
This condition occurs when the tissue muscle becomes weak enough that it allows the stomach to bulge up through the diaphragm. In some cases of hiatal hernia, it becomes unclear why this condition happens. But, the possible hiatal hernia causes include:
- Changes in the diaphragm with the age of an individual
- Having an abnormally large hiatus by birth
- Injury to this area mainly after any trauma or surgery
- Surrounding muscles get a continuous and intense pressure on them due to vomiting, coughing, straining while having a bowel movement, exercising or lifting hefty objects

WHAT IS THE CONNECTION BETWEEN GERD & HIATAL HERNIA?
It is widely known that a hiatal hernia can happen due to the presence of long-lasting GERD or GERD could be a symptom of a hiatal hernia.
As the GERD advances, it further weakens the lower esophageal sphincter (LES) – a muscular valve – and this causes the backflow of stomach acid into the esophagus thus creating discomfort. If GERD persists for a long time, it can cause a hiatal hernia.
A hiatal hernia happened when the part of the stomach pushes up into the chest cavity through the opening in the diaphragm (hiatus). Due to this, the lower esophageal sphincter becomes weak and its new position may keep it from closes tightly. A weak LES allows the acidic contents to move back to the esophagus, initiating chronic heartburn that finally leads to GERD.
WHAT ARE THE RISK FACTORS OF HIATAL HERNIA?
The condition occurs more frequently in women, persons who are obese or overweight, and people over than 50 or above.

HOW TO DIAGNOSE HIATAL HERNIA?
Normally, a hiatal hernia is diagnosed during a test or procedure that is performed to determine the underlying cause of heartburn or upper abdominal or chest pain. Here are these tests or procedures:
X-RAY OF THE UPPER DIGESTIVE TRACT:
The patient drinks a chalky liquid that coats and fills the interior lining of the digestive system and after that x-rays are taken. This coating allows the doctor to see the outline of the esophagus, the stomach, and the upper intestine.
UPPER ENDOSCOPY:
During the procedure of upper GI endoscopy, the doctor inserts an endoscope which is a thin, flexible tube having a light and camera down to the throat. This allows the doctor to examine the inside of the esophagus and the stomach and to check for any inflammation.
ESOPHAGEAL MANOMETRY:
This test is used to measure the rhythmic contractions in the esophagus when a person swallows. It is also used to measure the coordination and force that is exerted by the muscles of the esophagus.

HOW TO TREAT HIATAL HERNIA?
Most people having the condition don’t experience any symptoms and so they won’t need any treatment. But, if an individual experience recurrent signs and symptoms such as repeated acid reflux or heartburn, he/she may need hiatal hernia treatment that includes medication or surgery.
MEDICATIONS:
For acid reflux and heartburn, the physician may recommend these medications:
Antacids: These provide a quick relief while neutralizing the stomach acid. These include Rolaids, Mylanta, and Tums. The overuse of certain antacids can cause side effects such as kidney problems or diarrhea.
Medications for reducing acid production: These medications are known as H-2-receptor blockers and include ranitidine (Zantac), cimetidine (Pepcid) and nizatidine (Axid). The stronger versions of these medications are available by prescription.
Medications for blocking acid production and healing the esophagus: These medications are known as proton pump inhibitors and they are much stronger acid blockers as compared to H-2-receptor blockers. They provide enough healing time for the damaged esophageal tissue. OTC proton pump inhibitors include omeprazole (Prilosec, Zegerid) and lansoprazole (Prevacid 24HR). The stronger versions are available only in prescription.
SURGERY:
Sometimes, surgical treatment is required for hiatal hernia. Surgery is recommended when the medications are not enough to treat the symptoms of hiatal hernia or when the condition becomes complicated such as severe inflammation or narrowing of the esophagus.
Surgery is performed through different ways such as by pulling the stomach down into the abdomen and making the hiatus (opening in the diaphragm) smaller or by reconstructing the esophageal sphincter or by taking out the hernia sac.
There are times when the surgeon makes several small incisions in the abdomen and inserts a tiny camera and special surgical tools through these incisions. During this procedure, the surgeon views the images from inside of the body displaying on a video monitor and this is called laparoscopic surgery. Sometimes, the surgeon only makes a single incision in the chest wall and this procedure is called a thoracotomy.

CONCLUSION:
Hiatal hernia, at most times, doesn’t require medical treatment but if the symptoms are persistent and troublesome then the condition can be treated. The American board-certified gastroenterologist at GI Endoscopy Practice in NJ is providing the best treatment of hiatal hernia while customizing it according to the condition and needs of an individual patient.
To book an online appointment, visit our website or call us at 973-248-1550 for an immediate response.
Disclaimer: The information given in this article is purely available for informational and educational purposes only and shouldn’t be construed as medical advice. Always consult the physician for any medical concerns or regarding any medications or medical procedures.
You Might Also Enjoy...


What Is The Natural Treatment For H. Pylori Infection?

Constipation – How To Use The Best 5 Essential Oils?

How The Procedure Of Flexible Sigmoidoscopy Is Performed
Colon Polyps – A Complete Overview

